We all know sleep is important, which is why you should see a medical professional if you are having trouble getting to sleep or experiencing symptoms of any sleep disorders. Sleep disorders can be difficult to diagnose by visiting the GP and explaining your symptoms. A more conclusive way to diagnose a health condition or disorder caused by poor sleep is via a sleep study. Your doctor may refer you to a sleep specialist who can order either an at-home sleep study or a study conducted in a clinic.
What is a Sleep Study?
A sleep study, also known as a polysomnography, is non-invasive monitoring of the body overnight to diagnose sleep disorders. There are different forms of sleep studies depending on the symptoms and the suspected sleep disorder that a patient may be suffering from.
In-Lab Sleep Study
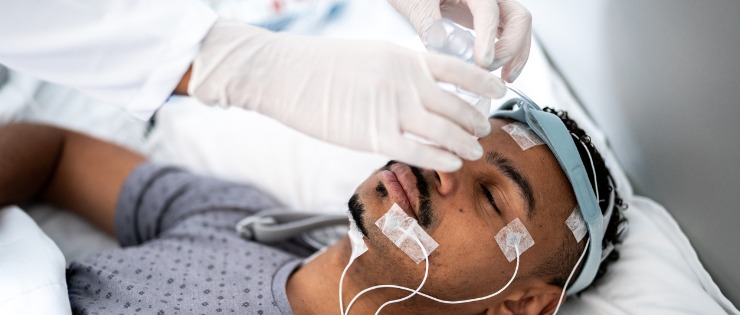
An in-lab sleep study is able to collect more information than an at-home study. An electroencephalogram (EEG) monitors cycles of REM and non-REM sleep, and measures brain waves; an electrooculogram (EOG) measures eye and chin movements that signal the different stages of sleep, an electrocardiogram (EKG) measures heart rate and rhythm, while chest bands measure respiration. Other monitors are used for recording oxygen and carbon dioxide levels in the blood and recording leg movement. All of the devices are non-invasive and not painful.
Information about eye movements, oxygen levels, snoring, heart rate and body movements are all recorded for analysis by a doctor at a later date. Sleep lab studies usually take place in a hospital or clinic. Different sleep studies available are used to diagnose different disorders.

Types of Sleep Disorders
There are several disorders that can be diagnosed after a sleep study.
Insomnia
Insomnia is a common sleep disorder - 14.8% of the Australian adult population have symptoms that could lead to a diagnosis of clinical insomnia. In a report commissioned by Sleep Health Foundation, 60% of people regularly experience at least one sleep symptom such as having trouble falling asleep or staying asleep. More women suffer from insomnia than men.
Restless Leg Syndrome
Restless leg syndrome is the urge to move your legs, usually because they feel uncomfortable, particularly in bed and while trying to fall asleep. The legs can have a burning, tingling, itching or aching sensation and can experience uncontrolled jerking movements. Moving the legs can reduce the symptoms but often stops sufferers from falling asleep. The syndrome can be caused by genetics, iron deficiency, dialysis, or peripheral neuropathies.
Sleep Apnea
Sleep apnea is a sleep disorder that causes breathing to stop and start, with stops generally lasting for 10 seconds or more during sleep. Symptoms of sleep apnea include heavy snoring, daytime fatigue, insomnia and multiple pauses in breathing during sleep. Obstructive sleep apnea is caused by the throat muscles relaxing too much during sleep so the throat is partly or completely blocked. Around 5% of Australians have sleep apnea, many undiagnosed. More males suffer from sleep apnea than females. A sleep study is the best way to diagnose sleep apnea.

Sleepwalking
Also known as somnambulism, sleepwalking is a behaviour disorder that occurs during sleep and results in walking during sleep. It’s most common in children, with most growing out of the condition by the time they are teenagers. Parents can usually direct their child back to bed without them waking.
Sleepwalking can be caused by irregular sleep hours, stress, medications and not enough sleep. It’s estimated that 5 in 100 children sleepwalk sometimes. A doctor may refer an adult sleepwalker for a sleep study if their sleepwalking is dangerous or to help improve their sleep.
Sleep Talking
Sleep talking, also known as somniloquy, is a form of parasomnia and is the most common sleep disorder, with 66% of respondents to a survey saying they have experienced sleep talking. Sleep talking causes people to call out or speak, either clearly or incoherently, during sleep. Sleep talking can be caused by illness, sleep apnea, a headache, a night terror or stress. Improvements in sleep hygiene can reduce the frequency and severity of sleep talking, but for some, a sleep study may diagnose a sleep disorder that may be causing the talking.
REM Sleep Behaviour Disorder
Also known as parasomnia, the REM sleep behaviour disorder involves body actions such as sudden movements or vocalisations. During the REM phase that starts 90 minutes after falling asleep, the muscles in the body usually enter a state of temporary paralysis. In people with the disorder, the paralysis is incomplete or absent, so the body can act out dreams, sometimes dramatically or violently. The person may wake and remember the dream, but not their movements. Up to four episodes per night are possible with each REM phase. RBD sufferers may go on to develop other neurological diseases such as Parkinson’s disease or Lewy body dementia.

In-Clinic Sleep Study
A sleep specialist can come from a variety of medical backgrounds. They may be pulmonologists (lung specialists), otolaryngologists (ears, nose, and throat), neurologists (brain and nerves), or psychiatrists (mental health). They may also be a general practitioner.
A sleep study conducted in a lab opposed to at home means patients can undergo a split night study where the first few hours are devoted to diagnosing a disorder such as sleep apnea. If the sleep specialist diagnoses obstructive sleep apnea, they can wake the patient and fit a positive airway pressure (PAP) device to see if the patient responds well to the device for the remainder of their sleep.
At-Home Sleep Study
The diagnosis of disorders like sleep apnea can be achieved through at-home sleep studies. The equipment involved in an overnight sleep test includes sensors that monitor sleep, breathing, pulse oximetry and pauses in breathing. The information is collected and stored. Once the equipment is returned, a sleep specialist can review the data and determine if a patient suffers from any sleep disorders.
At-home sleep study kits may vary slightly, but the bulk of them have the following equipment:
The benefits of at-home sleep studies over clinic or hospital studies are largely related to cost and comfort.
Cost
An at-home study is significantly cheaper than a sleep study conducted in a lab. Lab sleep studies require a professional to be in attendance and record their observations.
Comfort
Most people like to sleep in their own bed and in the privacy of their home, rather than sleeping in a strange environment with someone watching them.
Convenience
Staying at home for a sleep study means you don’t need to change your usual routine. Whether you’re a morning person or not, you’ll be home to have breakfast with your partner, get children off to school and yourself to work. When you’re in a lab study, you may need to make alternative arrangements if you have children to care for and will be driving home in peak hour traffic.

Risks of an At-Home Sleep Study
An at-home study may not be as accurate as a study conducted in a sleep lab with a professional. While at-home studies are valuable for diagnosing some sleep disorders, they may not be recommended for a patient suspected of having a serious life-threatening or chronic condition such as pulmonary disease, congestive heart failure or a neurological disorder.
If the results of an at-home sleep study are inconclusive or negative, a patient may be referred for a sleep study in a lab because the result is likely to be more accurate.
If you are consulting your healthcare professional about your sleep, ask about the possibility of being referred to a sleep specialist who may be able to organise an at-home sleep study. Certain hospital cover policies will cover your visit to a sleep specialist, so take a look at your options today