
Just as the world started to relax a little about COVID-19, a new pandemic hit the news. The World Health Organisation (WHO) announced a multi-country outbreak of monkeypox in July 2022. Since then there have been plenty of myths doing the rounds about what the monkeypox virus is and who are the most vulnerable.
What is Monkeypox?
Monkeypox is a zoonotic disease that can spread between animals and humans. In Africa, monkeypox is endemic and mostly found in tropical rainforest areas. Many people in Africa are infected through hunting, trapping and processing infected animals.
Symptoms of Monkeypox
The symptoms of monkeypox include:
- Fever
- Rash
- Back pain
- Swollen lymph nodes
- Muscle ache
- Sore throat
- Cough
- Nasal congestion
- Chills
- Exhaustion
- Headache
The rash lasts 2-4 weeks and varies in its appearance including:
- lesions with a flat base
- firm and raised papules that are painful
- vesicles that are filled with clear fluid
- pustules filled with pus
- scabs or crusts as the lesions heal
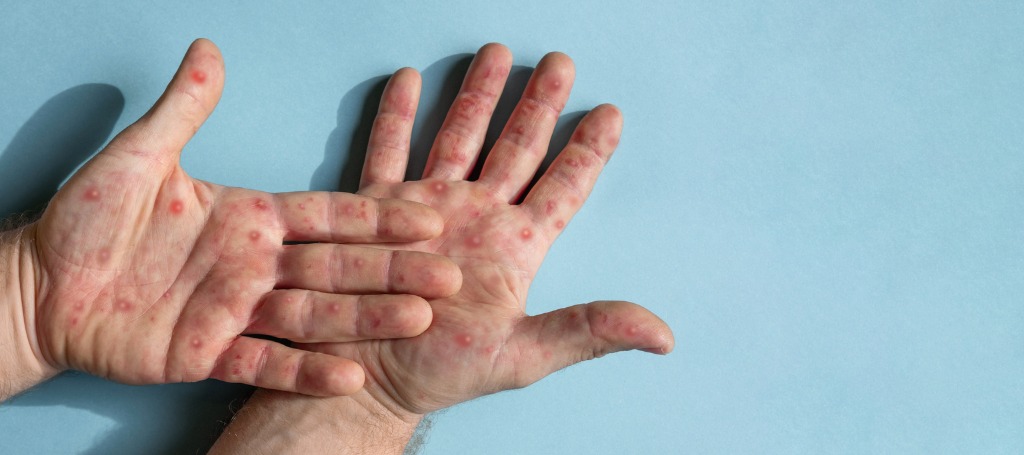
The symptoms vary from person to person. Some will experience flu-like symptoms with the rash appearing up to four days later, while others experience the rash first, or just the rash alone. There is no proven treatment for monkeypox. The illness usually lasts 2-4 weeks.
Monkeypox can sometimes be fatal but over 99% of people infected with monkeypox during the 2022 outbreak have survived. The most vulnerable are people with weak immune systems, children under the age of eight years, people who have eczema and women who are pregnant or breastfeeding.
The Clade 1 strain of monkeypox virus has a higher fatality rate of 10%. Clade I originated in the former Congo Basin (central Africa) and Clade II originated in western Africa. Clade IIb is the group of variants circulating in the 2022 global outbreak.
Transmission of Monkeypox
One of the myths around monkeypox relates to how contagious it is. Luckily it’s nowhere near as contagious as COVID-19 or measles. Monkeypox spreads through close or intimate contact. Skin-to-skin contact is the most common way people are infected but it can occur via a few means:
- Touching a monkeypox rash or the scabs
- Touching fabric such as bedding, a towel or clothing that has been used by an infected person
- Contact with respiratory secretions
- All forms of sexual intercourse or touching the genitals of an infected person
- Hugging, kissing, face-to-face contact
- Touching objects that have been used by an infected person and not yet disinfected

It’s also possible for monkeypox to pass from an infected animal to human through a scratch or bite, or preparing and eating meat.
Research is being done into whether the virus can be spread by someone who has no symptoms, when respiratory secretions are most likely to spread the virus, therefore when bodily fluids can infect another person.
People should isolate themselves from others until their sores are completely cleared.
2022 Outbreak
During this outbreak, over 68,000 people in 100 countries have contracted monkeypox. Around 25,000 of these have been recorded in the US. At the peak in August, 736 cases were recorded a day but by late September that number had dropped to just over 100. Australia has had 136 cases in total, with half recorded in Victoria. Some health experts are saying that it’s unlikely that monkeypox will be eliminated from many countries following this year’s outbreak while others are more optimistic.
Vaccination Against Monkeypox
People concerned about catching monkeypox have enquired about getting a vaccine. Vaccines developed against smallpox are being used to prevent monkeypox infections.
Only people who are most at risk of getting monkeypox are recommended to get vaccinated. Those people include:
- Medical staff who perform testing on people expected to have been infected with the monkeypox virus
- Laboratory staff who handle the test cultures
- People who have been exposed to the virus - if given soon after it may prevent the onset of symptoms or reduce the severity
- People who have multiple sexual partners
Monkeypox Myths
#1 Monkeypox is a new disease
The monkeypox virus was first discovered in 1958 in a Danish animal centre. The first human case was detected in the 1970s. Monkeypox has been circulating in Africa, particularly in the Democratic Republic of the Congo since then. Monkeypox is considered endemic in Africa. The US recorded a small outbreak in 2003 that was linked to imported pet prairie dogs. This year’s outbreak is the first one that has many countries recording cases that aren’t linked to international travel or contact with animals.
#2 Monkeypox is a highly contagious virus.
Monkeypox has a reproduction rate R of 0.85. The Omicron variant of COVID-19 is 8.2 so Omicron is far more contagious. A virus isn’t considered a pandemic if the R rate is less than 1. According to WHO, the longest chain of transmission for monkeypox is six generations (six people away from the original infected person).
#3 Monkeypox doesn’t infect heterosexuals
Amongst the US’ 22,000 cases, around 98% have been homosexual or bisexual men. But heterosexual people of any age or gender can be infected through close or intimate contact. In comparison to the US, most African cases have been seen amongst heterosexual individuals.
#4 You may catch monkeypox in a crowded room
The virus that causes monkeypox can survive on surfaces especially when they’re in dark, cool environments with low humidity. It is possible that you could catch monkeypox from a contaminated surface but the likelihood of that happening is low. Most people are being infected through direct skin to skin contact.

#5 If you’ve had chickenpox or the vaccine, you have some immunity against monkeypox
Chickenpox and monkeypox are two different families of viruses so you have no protection against monkeypox. Shingles also won’t provide any protection against being infected with monkeypox.
#6 If you’ve had the smallpox vaccine as a child, you’ll have some immunity against monkeypox
Smallpox and monkeypox are in the same family of viruses so the smallpox vaccine offers some protection. However, immunity wanes with time so if you had the injection as a child, it’s unlikely you will be protected.
#7 Anyone can have the smallpox vaccine to protect against monkeypox
The smallpox vaccine isn’t considered safe for people who are immunocompromised or have skin conditions like eczema.
#8 Monkeypox is only found in monkeys and humans
While a monkey was the first animal found to have the virus, many animals can be infected by the virus. Monkeypox has also been found in anteaters, dogs, squirrels, giant-pouched rats, prairie dogs, shrews, and even hedgehogs. It is unknown if other animals can be infected but it’s thought that reptiles and birds are unlikely to be infected because they haven’t caught other orthopoxviruses.

Need Healthy
Lifestyle Benefits?
We've got you covered
Call 1300 134 060 or Get a quote
Treatment of Monkeypox
Monkeypox is genetically similar to smallpox so antiviral drugs used to treat smallpox are being used on people with monkeypox infections.
It is possible for bacterial infections to occur while monkeypox lesions are healing. To reduce the chance of infection and to prevent scarring, people should try not to scratch their lesions. Antibacterial washes a few times per week in the shower can help rescue the risk.
While there are no treatments specifically used to tackle Monkeypox symptoms, you may need to consult your doctor for advice or medication. In some cases, Monkeypox can result in a trip to the hospital. In the event of an infection, certain HIF combined cover policies will ensure you get the treatment you need.