Do you skip brushing and flossing sometimes and think you’re just risking a filling? If only your poor hygiene habits were that benign. You should be more concerned about periodontal disease.
Chances are you won’t know you have until it’s done irreversible damage to your gums, teeth and jaw bone. Find out what signs you should look out for, the causes and treatment available for a disease that can do so much damage.
What is Periodontal Disease?
Periodontal disease or gum disease as it’s often called is when an infection causes inflammation of the gums, destruction of the periodontal ligament and supporting bone. In advanced cases, teeth can loosen and fall out because of the gum movement and loss of bone.
Periodontal disease or gum disease affects around 20-50% of the global population. In the US, more men (56.4%) than women (38.4%) experience periodontal disease. In the US, 47.2% of adults over the age of 30 have a form of periodontal disease according to the Centers of Disease Control and Prevention (CDC).
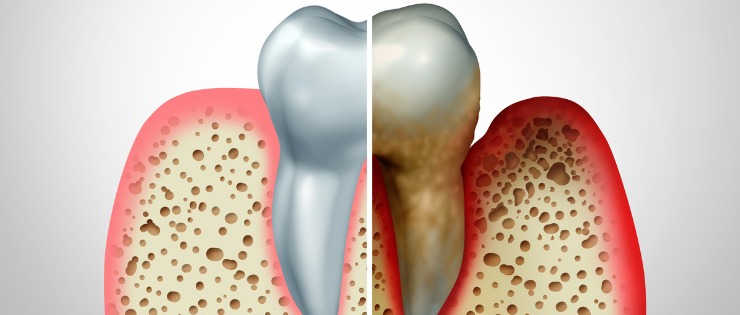
What Causes Periodontal Disease?
There’s a wide range of factors that contribute to periodontal disease. Some factors are lifestyle related and can be avoided, but many can’t.
Advancing age is one of the biggest factors in periodontal disease. In the US, it’s estimated 70.1% of people aged 65 and older have mild, moderate or severe periodontal disease. Even from the age of 30, it’s estimated that around 50% of the population is impacted.
Dentists have found periodontal disease to be hereditary, so if a parent or sibling has had it, you’re at greater risk than others with no family history. Individuals with immunodeficiencies such as AIDS are at higher risk. Some medications that cause a dry mouth can increase the risk. Women taking oral contraceptives or who are pregnant also have a higher chance of developing periodontal disease.

Dental problems such as defective fillings, a dental bridge that doesn’t fit correctly and crooked teeth are all risk factors for developing periodontal disease. Poor oral hygiene has an enormous influence on developing the disease.
What are the Stages of Periodontal Disease?
Some dentists say there are four stages of periodontal disease, while others believe it’s three with the middle stages combined.
Gingivitis
Slight periodontal disease
Moderate periodontal disease
Advanced periodontal disease
Stage 1 - The Role of Gingivitis in Periodontal Disease
Gingivitis is the first stage of periodontal disease and is the name given to red, swollen and bleeding gums. Inflammation of the gums is common and fairly harmless in the early stages.
This is the only stage of periodontal disease that’s reversible. When the inflammation spreads to other parts of the periodontium that gingivitis becomes the more harmful periodontal disease.
The build-up of plaque (a thin film of bacteria) near the gum is a common cause of gingivitis so the best way to avoid it is maintaining good oral hygiene.
Brushing and flossing regularly reduces the bacteria in the mouth and plaque around the gum and teeth. But gingervitis rarely causes pain or any other symptoms, so it often goes undetected until a visit to the dentist.
You are more likely to develop gingivitis from:
Smoking
Metabolic diseases such as diabetes
Hormonal changes during pregnancy
Taking medications that suppress the immune system, and
Medications for cardiovascular disease
Improved oral hygiene and regular visits to the dentist can help control gingivitis and reduce the chance of it becoming periodontal disease.
If left untreated gingivitis can cause large gum pockets around the teeth where the gum has pulled away. As the pockets deepen, it is harder to reach the bacteria with the toothbrush, and the bacteria builds up on the root and neck of the tooth where it can harden.
The bacteria and tartar in the pocket can cause further inflammation which can attack the soft tissue and bone supporting the teeth. It’s important to treat gingivitis, so it doesn’t develop into more serious problems.
Stage 2 - Slight Periodontal Disease
The start of stage two is when irreversible damage can begin. The infection has continued and now spread to the bone. In some people, the bacteria can become quite aggressive resulting in more damage.
It’s still not obvious to many individuals they have stage two periodontal disease but they may notice bleeding, swollen or red gums or bad breath.
Stage 3 – Moderate Periodontal Disease
During this stage, the bacteria has moved from 4-5 mm below the gum (in stage two) to 6-7 mm. The bacteria is damaging bone but can also enter the bloodstream and attack the immune system. They need deep cleaning of the roots by a dentist to remove the bacteria and reduce the chance of teeth moving in the gums.
Stage 4 – Advanced Periodontal Disease
The last stage of the disease, if left untreated, can result in bone loss. The signs of advanced periodontal disease are unmissable with increased bleeding, sensitivity, pus in the gums, loose teeth, pain when eating and bad breath.
If people don’t seek treatment now, they may experience gaps between their teeth, recessed gums, tooth loss and serious health problems caused by the infection.
The treatment may include surgery, lasers, and antibiotics.
What are the Symptoms of Periodontal Disease?
Many people aren’t aware they have periodontal disease until they see their dentist but there are some warning signs. If you recognise any of the following indicators, make an appointment with your dentist to have it checked out.
Red or swollen gums
Sore or bleeding gums
Bad breath or bad taste that won’t go away
Pain when chewing food
Loose teeth
Teeth sensitivity
Gaps between the gum and teeth
Any change in the way your teeth fit together when you bite
Any change in the fit of partial dentures
Diagnosis of Periodontitis
At each appointment, your dentist will check for signs of gingivitis as a warning sign of stage one periodontitis. Your dentist may use a probe to measure the pockets around teeth. The normal depth of a healthy gum pocket is 1-3 mm and anything deeper is a concern.
A dentist routinely uses x-rays to check below the gum line including bone health. A dentist may ask patients about their medical history to check on risk factors such as smoking, and diabetes.
If there are any concerns, a dentist may refer patients to a periodontist, a dentist who specialises in the diagnosis and treatment of periodontal disease.
If you have risk factors for periodontal disease or you’ve had gingivitis before, you may benefit from seeing your dentist more regularly. A professional check on the health of your gums and to clean off any plaque or tartar build-up can reduce the chance of the disease taking hold.
What Treatments Are Available for Periodontal Disease?
The earlier periodontal disease can be detected, the easier it is to treat. The most important treatment is to remove the bacterial plaque and hard tartar from around the teeth.
Scaling teeth and root planing or deep cleaning is often enough to keep the disease from getting worse and causing more damage to the gums, teeth, tissue and bone.
However, if the disease is advanced and the cleaning can’t be completed in the dentist’s chair, a patient may be recommended for surgery. During surgery it’s possible to clean the root surface of teeth, repair and regenerate the soft and hard tissues and replace missing teeth with dental implants.
Once the inflammation has subsided some patients may need occlusal bite therapy to deal with loose teeth, and dental problems caused by clenching and grinding.
A dentist may recommend that a patient quit smoking to improve their oral health. But the most important treatment is for patients to change their oral hygiene habits. Without committing to brushing twice a day, regular flossing and routine dentist visits for a check-up and professional clean, their dental problems will likely persist.
FAQs About Periodontal Disease
The more questions people ask to improve their knowledge of periodontal disease, the greater the chance of them avoiding it.
Can you fix periodontal disease?
It depends on when periodontal disease is discovered and how much, if any, damage has occurred. Damage to tissue and bone around teeth can’t be undone, but treatment and ongoing monitoring from your dentist can stop periodontal disease from doing more damage.
What happens if periodontal disease goes untreated?
If left untreated, periodontal disease causes deep gum pockets around teeth which lets plaque and tartar to build-up in areas you can’t clean with your toothbrush. The tartar can damage tissue and cause bone loss leading to loose or fallen teeth.
How do you get periodontal disease?
Poor teeth hygiene is one of the most common causes of gingivitis and periodontal disease. Brushing and flossing your teeth twice a day keeps the plaque under control and stops the bacteria getting deep in the gum where your toothbrush can’t reach. Other factors include old age, medications, health and other dental conditions.
How does regular brushing stop gum disease?
Humans have around 600 species of bacteria in their mouth, so it’s a conducive environment for growing disease-causing bacteria in biofilm called dental plaque. Daily brushing and flossing disturbs the biofilm and stops the bacteria moving into hard to reach periodontal pockets around the teeth.
What are some of the early warning signs of periodontal disease?
Any change in the appearance of your gums can be a warning sign that you’re in the early stages of periodontal disease. Not all gum changes are linked to periodontal disease but if you have other risk factors such as over the age of 65, get it checked out by your dentist.
If you notice pain or sensitivity with any of your teeth while eating, it’s not a sure sign you have the disease, but there’s a chance.
Make an appointment to see a dentist as soon as you notice any changes with your mouth so you can get a diagnosis and begin treatment if required.